Rheumatoid arthritis is a chronic disease characterized by joint pain, swelling and stiffness that eventually leads to loss of joint function.
It is an autoimmune disorder as the immune system attacks the healthy tissues of the joints due to its hyperactivity.
Symptoms of rheumatoid arthritis
Like many other autoimmune diseases, it is characterized by fluctuating disease activity. Patients with this disease present phases of remission in which the disease stabilizes and phases of relapse in which the disease symptomatology worsens.
Among the characteristic symptomatology of rheumatoid arthritis, the following stand out:
- Swelling, joint pain both at rest and in movement
- Fatigue and lack of energy
- Functional loss of joints
- Joint stiffness especially noticeable in the mornings
- Loss of appetite
- Inflammation can be systemic, also affecting the skin, eyes, lungs, heart and blood vessels, among other organs and tissues.
It can affect various joints, but the most frequent are the hands, wrists and feet.
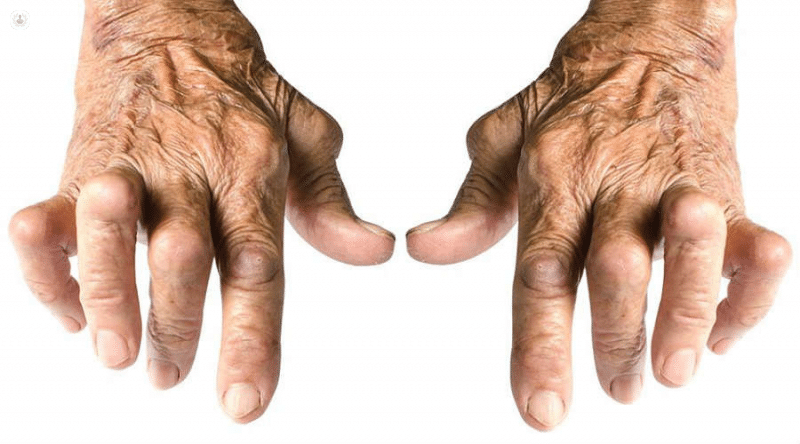
Causes of rheumatoid arthritis
It is a complex and multifactorial condition whose exact causes are still under investigation, although it is recognized that genetic, environmental and immunological factors are involved. Risk factors include:
- Age: most cases occur in middle age, but it is not a disease exclusive to this age group.
- Sex: the prevalence of the disease is higher in women (about 0.8%) than in men (about 0.2%) in people over 20 years of age.
- Smoking: smoking is considered a risk factor, especially if you have a genetic predisposition to develop rheumatoid arthritis.
- Obesity: not only is it considered a risk factor, but it can also limit the improvement of the disease.
- Viruses: sometimes certain viral infections can trigger the disease.
- Stress: not only is it among the risk factors, but it can influence the body's inflammatory response, worsening the symptoms of the disease.
- Genetics: Genetics can increase the likelihood that your immune system will react to exposure to various environmental factors. Therefore, although genetics does not determine the presence or absence of this disease, it can predispose you to a greater or lesser extent to develop it.
Genetics and rheumatoid arthritis
Over the years, research has identified several genes that are associated with an increased risk of developing rheumatoid arthritis.

- HLA-DRB1: This is one of the genes most closely linked to rheumatoid arthritis. It is part of the major histocompatibility complex (MHC) class II, which plays a crucial role in the immune response. Specific variants of this gene are associated with an increased risk of this pathology and may influence the severity of the disease.
- PTPN22: encodes a protein involved in the regulation of signaling in immune cells. Variations in this gene have been associated with an increased risk of developing several autoimmune diseases, including rheumatoid arthritis.
- STAT4: This gene is involved in signaling pathways that regulate immune system activation. Variants of the STAT4 gene have been linked to an increased risk of rheumatoid arthritis and other autoimmune diseases.
- TRAF1–C5: The genetic region that includes these two genes, TRAF1 and C5, has been associated with rheumatoid arthritis. Although the exact mechanism is still unclear, alterations in this region could affect the inflammatory or autoimmune response.
- TNFAIP3: This gene, which is related to the regulation of the inflammatory response, has been implicated in susceptibility to rheumatoid arthritis. Mutations or variants in this gene could play a role in the inappropriate activation of the immune response in this pathology.
- CCR6: The CCR6 gene encodes a receptor present on certain immune cells, and variations in this gene have also been linked to an increased risk of developing rheumatoid arthritis.
Thanks to the DNA TEST If you are already genotyped, you can find out your genetic predisposition to develop rheumatoid arthritis along with many other diseases, find out and be part of the community! If you are already genotyped, upload your DNA data.